
Pr Loïc Ysebaert
Leukemia and immune cell resistance to targeted therapies in chronic lymphocytic leukemia (cll)
Chronic lymphocytic leukemia (CLL) is the second most common form of non-Hodgkin’s B lymphoma. This disease is characterized by microenvironment-dependent survival/proliferation of CLL cells in secondary lymphoid organs and accumulation of quiescent leukemic B cells in the blood.
The clinical management of first-line and relapsed patients has been revolutionized by the development of targeted oral therapies, including ibrutinib (a BTK (Bruton Tyrosine Kinase) inhibitor), and venetoclax (a BCL-2 inhibitor) in combination or not with therapeutic anti-CD20 antibodies. Despite long periods of remission, 2 mechanisms of resistance always develop: clonal selection with acquired mutations of the BTK/PLCg2 and BCL2 genes, or abrupt transformation (unpredictable, independent of the above-mentioned mutations) into aggressive lymphoma (Richter syndrome, RT). In a prospective longitudinal cohort of patients treated with ibrutinib monotherapy, our results show that only 60% of patients who progressed on treatment (> 3 years of ibrutinib) acquired one of these 3 mutations that could account for the relapse. This study demonstrates the wide variety of genomic alterations that allow resistance to ibrutinib. Nevertheless, at the cellular level, the transcriptomic programs regulated by these mutations are not identified.
Objectives of research project:
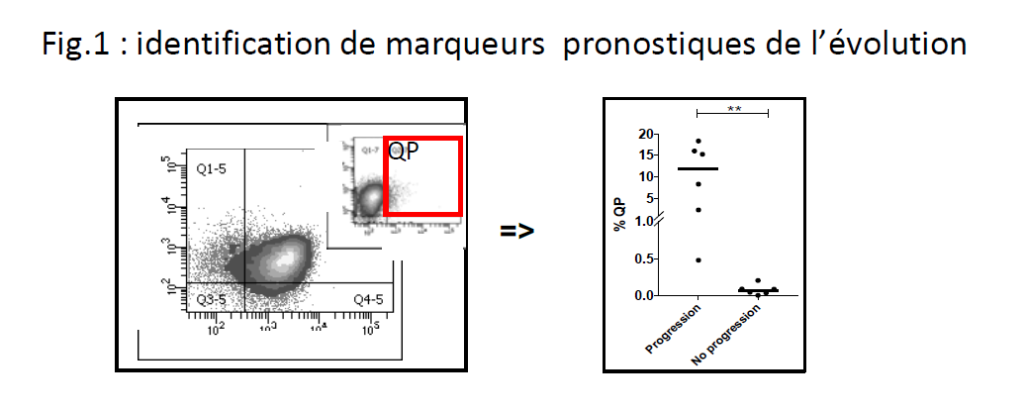
- to identify prognostic markers of CLL patients’ progression under targeted therapies to better anticipate progression or transformation
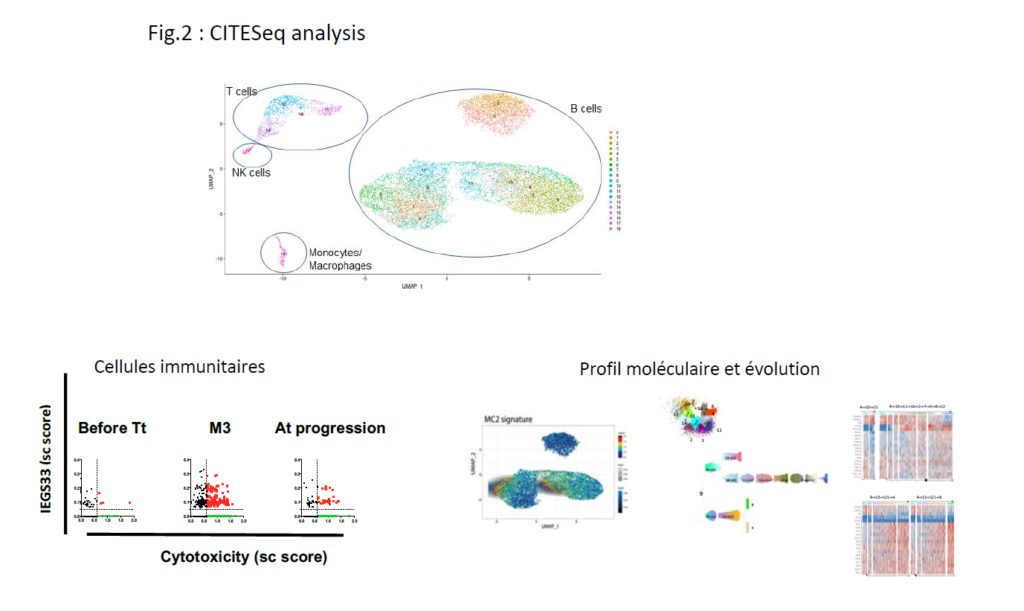
- using a high-tech single cell sequencing approach (CITESeq): to understand the physiological state of normal immune cells, to identify the genetic signature of resistant leukemic cells and to define new therapeutic targets
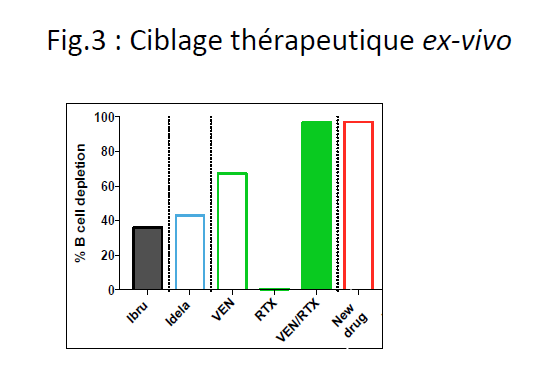
- validate the targets identified by CITESeq by ex-vivo therapeutic screening and propose the most appropriate treatment for each case
Parternships and funding: :
IUC/CRCT (Projet Demetar ; AO Translationnel)
